Viral Vaccine Immunology
What happens after you are injected with a viral vaccine? And which viral vaccine type is best?
(Note that I’m going to be talking about viral vaccines ONLY.)
First of all, there two basic types of viral vaccines: live attenuated vaccines (LAV) and inactivated (killed) vaccines.
LAV contain a vaccine virus that is a weakened version of the natural disease-causing virus. Inactivated vaccines use a killed version or a part(s) of the natural virus.
The body’s response to the vaccine virus in relation to the natural disease-causing virus has to do with the type of vaccine being administered, as well as how similar the vaccine virus is to the natural virus.
I’m going to go ahead and stop saying “vaccine virus”, and start calling this the “antigen”. An antigen is something foreign (in this case) that the body makes an immune response to, or something that’s the target for an immune response.
An inactivated vaccine contains all of the antigen needed to induce an immune response in the injected dose. Once it is injected into the muscle, the immune system begins to respond to this antigen. The LAV works a bit differently. There is only a very tiny amount of live weakened virus, and it must use the host body’s cells to reproduce in order to create the proper immune response. Once a LAV is injected into the muscle, the antigen migrates to the appropriate tissue in order to begin replication. The “appropriate tissue” in this case would be the tissue the natural virus would normally infect and replicate in.
Because the vaccine virus is so similar to the natural virus in LAV, these vaccines create an immune response virtually identical to the natural infection. The inactivated vaccine’s response is similar, yet one drawback is that immune stimulation occurs at the site of injection and not at the site of natural viral replication.
Some inactivated vaccines contain an adjuvant. An adjuvant is something added to the vaccine (most often an aluminum salt), and is used to help create a stronger immune response by activating the immune system or directing the antigen to the appropriate immune cells. If the vaccine has an adjuvant attached, the adjuvant dissociates and begins enhancing the “danger” signals already being picked up by the body’s first line of defense: the innate immune system.
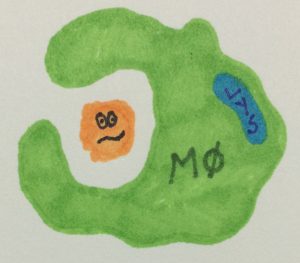
Macrophages (Mφ) and dendritic cells (DC) are cells of the innate immune system that “see” this antigen first. These types of cells have special receptors that recognize antigen as non-self and thus, as danger to the body. With this danger comes the flooding of more of these cells, several other types of immune cells, and the generation of inflammation.
The many Mφ recognize the antigens as foreign invaders and engulf them. Once inside, the antigen is chopped up into smaller pieces and then displayed on the Mφ surfaces. The Mφ send out signals to increase inflammation and bring leukocytes to the site of the antigen. Macrophages present the antigen pieces to the leukocytes.
For more on this: The beginning innate immune response to a microbe.
Remember I said LAV travel to the site of natural infection? This response and immune stimulation, including inflammation, would occur there. An inactivated vaccine response occurs at the injection site. This makes the site for non-live vaccines much more important than for live vaccines. Injection must be given in a place where patrolling DC are in larger quantities. Dendritic cells are always on patrol in the body, and found in especially high numbers in the vascularized muscle tissue. Therefore inactivated vaccines are injected into the muscle for greater immune response.
Once DC encounter the antigen, they can engulf it, undergo a brisk maturation, and then migrate through the lymphatic system to local lymph nodes. There, they encounter B and T lymphocytes (B cells and T cells).
The DC are able to provide the T cells with antigen-specific “danger” signals (cell-mediated immunity). T cells subsequently become activated and CD4+ T helper (Th) cells send out growth factors and signals to generate B cell responses and CD8+ cytotoxic T lymphocytes (CTL) responses. CTL can kill viral infected cells and release anti-viral chemicals. The B cells proliferate and differentiate into antibody-secreting plasma cells or memory B cells. Antibody-secreting B cells release antibodies capable of binding that specific antigen (humoral immunity).
So which type of vaccine creates the “best” response?
The response to a LAV is almost identical to the response the body would make to the natural virus. Research shows that the immune system cannot tell the difference between the two responses.3 LAV are also often effective with just one dose (except for the live oral vaccines).
Several doses are needed of inactivated vaccines to yield full protective immunity. The first dose “primes” the immune system. One or two more doses are needed before there is full protection. With this type of vaccine, it is also important to maintain the proper schedule when getting vaccinated. There must be a minimal time of 3 weeks between the primary dose and the following dose. This allows for successive waves of antigen-specific responses. Following those, you must wait 4 months before getting the following booster. This allows for affinity maturation of memory B cells, which leads to a higher secondary responses. And antibody titers often wane over time, so boosters are needed to maintain protection with inactivated vaccines.
In comparison, LAV usually maintain a longer lasting antibody response. This is due to the persistence of antigen within the host.
Live attenuated vaccines are the current ideal vaccine type. They generate strong and long-lasting responses. The inactivated vaccines, though, when administered properly and following the correct time schedule, are also very powerful immune system stimulators and do offer a huge amount of protection from disease.
So what’s the best vaccine? The one that keeps you from getting sick! Go get vaccinated.
Resources:
1. Siegrist, Claire-Anne. Vaccine Immunology. Elsevier Vaccine Immunology. Link.
2. World Health Organization. www.who.int
3. Immunisation Advisory Center. www.immune.org
8 thoughts on “Viral Vaccine Immunology”
Comments are closed.




Thats the most asinine rambling garbage I’ve ever had the misfortune of reading. Educated and intelligent people vaccinate because they understand that they don’t understand everything, but trust in the scientific process and take the advice of those who have been proven credible and do understand certain things that the aforementioned intelligent people don’t.
Educated people who lack intelligence but try to compensate with over inflated egos don’t vaccinate becuase surely no-one could know anything they can’t understand themselves, and big words sound scary.
Except for the dead ones, of course…
In fact, one of your own sources states:-
“The evidence does not indicate a causal relation between DPT vaccine or the pertussis component of DPT and infantile spasms.”
And:-
“Evidence does not indicate a causal relation between DPT vaccine or the pertussis component of DPT and hypsarrhythmia.”
And:-
“There is insufficient evidence to indicate a causal relation between DPT vaccine and aseptic meningitis.”
And:-
“On the basis of a review of the evidence bearing on this relation, the committee concludes that the range of excess risk of acute encephalopathy following DPT immunization is consistent with that estimated for the NCES: 0.0 to 10.5 per million immunizations.
There is insufficient evidence to indicate a causal relation between DPT vaccine and permanent neurologic damage.”
If you ever cross the road or carry your child in a car your risk of causing injury is massively greater. You really need to understand statistical likelihood of injury.
I will believe you if you can explain what the title of this article you posted means: “Kinetics of asthma- and allergy-associated immune response gene expression in peripheral blood mononuclear cells from vaccinated infants after in vitro re-stimulation with vaccine antigen”
Given that there is no Mercury in any vaccine (and there never has been – learn the difference between elements and salts), that the first study you cite actually simply recommends monitoring very young babies for 48 hours, that you would get more Formaldehyde from eating a pear (average 1200ug) than from the entire vaccination schedule, that yeast protein is essential for making bread and is the main ingredient in Quorn, and that mono-sodium glutamate is commonly found in far, far higher doses in chinese takeaway food I have to conclude that you are wilfully ignorant.
Why do you come here to an immunologists page and post things that a lay person can easily refute? It would be amusing if it didn’t endanger innocent children.
Causation has been proven in a number of areas that remain undisputed. Vaccines cause Sleep Apnea and Bradycardia [1] and the CDC says that they produce a 7-fold increased risk of developmental neurologic impairment for children vaccinated in the first 30 days of life [2]. We also know that vaccines cause Chronic Arthritis, Acute Arthritis and Encephalopathy [3] and that they tend to predispose us to Asthma and a lifetime of Allergies [4]. Please keep that in mind…
References:
1. Incidence of apnoea and bradycardia in preterm infants following DTPw and Hib immunization: A prospective study, Journal of Paediatrics and Child Health, Volume 33, Issue 5, pages 418–421, October 1997: http://onlinelibrary.wiley.com/doi/10.1111/j.1440-1754.1997.tb01632.x/abstract;jsessionid=5D10A874F54ED01C1B1AE0387A4988B1.f02t04
2. Increased risk of developmental neurologic impairment after high exposure to thimerosal-containing vaccine in first month of life, CDC, Verstraeten, Thomas M., MD, NIP, Division of Epidemiology and Surveillance, Vaccine Safety: http://thinktwice.com/CDC_quashed_study.pdf
3. Adverse Effects of Pertussis and Rubella Vaccines: A Report of the Committee to Review the Adverse Consequences of Pertussis and Rubella Vaccines, Washington DC National Academies Press, National Institute of Health, 1991: http://www.ncbi.nlm.nih.gov/pubmed/25121241
4. Kinetics of asthma- and allergy-associated immune response gene expression in peripheral blood mononuclear cells from vaccinated infants after in vitro re-stimulation with vaccine antigen, Elsevier, February 2008,
https://app.box.com/s/vgf1widrldfdu4t3gxsmfjdcgq521ipy
The Vaccine Injury Compensation Program has compensated upwards of 3500 families of primarily children who have been permanently vaccine injured or killed to the tune of just under 3 billion dollars. If we extrapolate those injuries and deaths across the global population we can estimate that at least 85,000 children have been seriously and permanently injured or killed by vaccines.
Of course we also know that the Vaccine Injury Compensation Program represents perhaps only 10% of those actually injured meaning close to 1 million children have been permanently injured or killed by vaccines.
Significantly, if you put the amount of mercury added to the immunization schedule as a result of the CDC-recommended seasonal and (in 2009) H1N1 flu shots** on one side of a scale, and the amount of mercury that was subtracted from that schedule by reformulating early childhood vaccines without Thimerosal on the other side, the total amount of mercury added far outweighs the amount of mercury subtracted. Currently, the actions taken by the vaccine manufacturers, the FDA and the CDC have increased the possible maximum childhood exposure to mercury from vaccines to twice the level that triggered the 1999 call to remove mercury from all vaccines as soon as possible.
In just the first 6 years of life we inject the following chemicals and elements into our children’s bodies which then encounter the adaptive immune system completely bypassing the innate immune system:
• 17,500 mcg 2-phenoxyethanol (antifreeze)
• 5,700 mcg aluminum (a known neurotoxin)
• Unknown amounts of fetal bovine serum (aborted cow blood)
• 801.6 mcg formaldehyde (carcinogen, embalming agent)
• 23,250 mcg gelatin (ground up animal carcasses)
• 500 mcg human albumin (human blood)
• 760 mcg of monosodium L-glutamate (causes obesity & diabetes)
• Unknown amounts of MRC-5 cells (aborted human babies)
• Over 10 mcg neomycin (antibiotic)
• Over 0.075 mcg polymyxin B (antibiotic)
• Over 560 mcg polysorbate 80 (carcinogen)
• 116 mcg potassium chloride (used in lethal injection to shut down the heart and stop breathing)
• 188 mcg potassium phosphate (liquid fertilizer agent)
• 260 mcg sodium bicarbonate (baking soda)
• 70 mcg sodium borate (Borax, used for cockroach control)
• 54,100 mcg of sodium chloride (table salt)
• Unknown amounts of sodium citrate (food additive)
• Unknown amounts of sodium hydroxide (Danger! Corrosive)
• 2,800 mcg sodium phosphate (toxic to any organism)
• Unknown amounts of sodium phosphate monobasic monohydrate (toxic to any organism)
• 32,000 mcg sorbitol (Not to be injected)
• 0.6 mcg streptomycin (antibiotic)
• Over 40,000 mcg sucrose (cane sugar)
• 35,000 mcg yeast protein (fungus)
• 5,000 mcg urea (metabolic waste from human urine)
• Other chemical residuals
(From the book, “What The Pharmaceutical Companies Don’t Want You To Know About Vaccines” – By Dr Todd M. Elsner)
Fools following fools vaccinate. Intelligent, well researched people don’t. Unvaccinated children are ALWAYS healthier than the vaccinated.
Hi, it is truly a nice post and thanks for sharing it with us. I’ve learned a lot about the viral vaccines.
http://www.creative-bioarray.com/