Chickenpox vaccine is great, but it’s got us 30+ year-olds getting shingles. Here’s why…
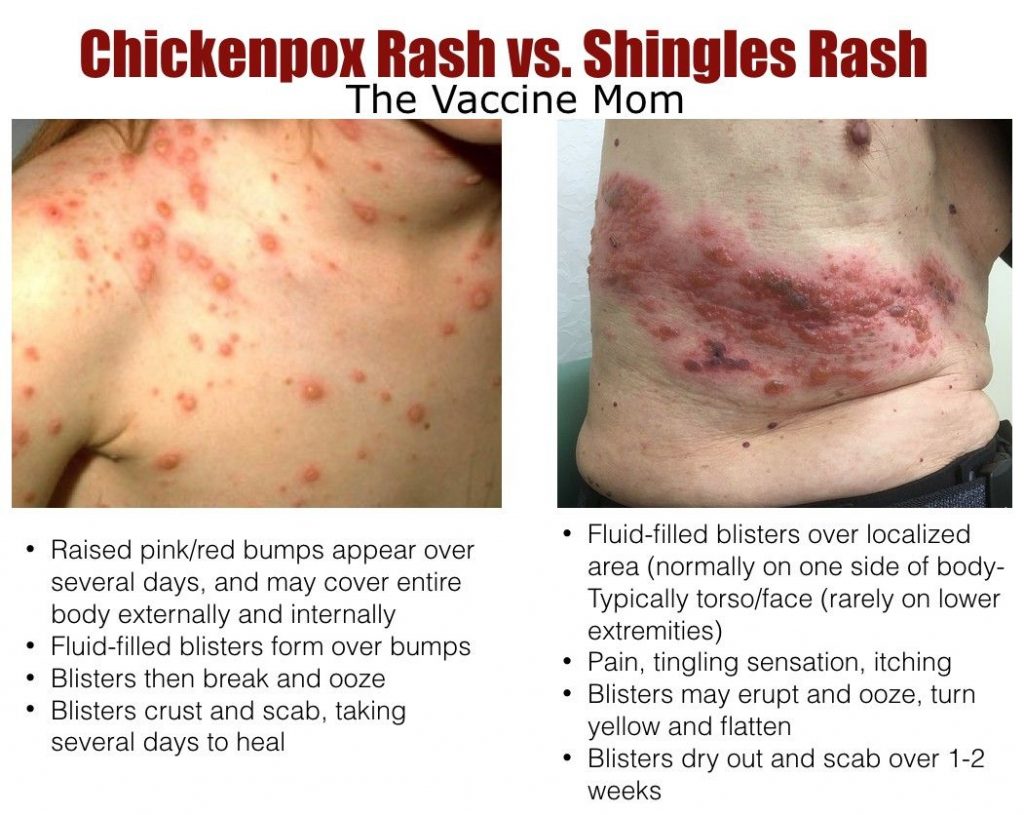
Once you’ve had the natural chickenpox virus in your body the virus goes dormant in your nervous system until possibly one day when you’re under a time of extreme stress/immunocompromise and the virus reactivates. Reactivation of the varicella virus (chickenpox) causes shingles (zoster).
Since these kids have never had the chickenpox virus, theoretically they won’t get shingles later in life. That’s assuming the vaccine is effective, most everyone has been vaccinated, and these children do not get the wild virus.
We can’t expect that all children will be vaccinated, however, the chickenpox vaccine is so effective that the seroconversion rate (when antibodies develop to a detectable level in the blood) is around 95% in healthy children.(2) That means the vaccine works pretty well, so it should help create good herd immunity if most children are vaccinated, and thus, aid in the prevention of shingles for the uninfected/vaccinated later in life.
So, simplified–if you’ve had chickenpox you are able to get shingles. If you’ve never had chickenpox you are not able to get shingles. If you’ve had the vaccine, you’ve never had chickenpox so you shouldn’t get shingles.
So what does that mean for our generation (assuming you’ve never had the chickenpox vaccine)?
That means it’s possible that you’re more likely to get shingles, and get shingles at a younger age. Why?
Shingles is thought to occur when antibodies to the natural chickenpox virus start to decline. Scientists are finding that re-exposure to chickenpox as an adult can help to act as a booster to keep antibody memory to chickenpox strong in those who have already had chickenpox. These “boosters” keep the incidence of shingles down, especially for those of under prime shingles age (50+ years).
So, how do you get re-exposure to chickenpox?
Simply, just be around children who have the chickenpox.
It has been found that people between the age of 15-44 have a reduced rate of shingles in coincidence with an increase in chickenpox in children under five.(4) And when there has been a child in the household with chickenpox, there is a reduced risk of shingles for the associated adults for around 20 years thereafter. Aka, more contact with sick children leads to a significantly lower incidence of shingles in adults. (3)
The problem is, if our children are vaccinated against the chickenpox, there will be no re-exposure for adults and thus, no immunity boosts. That means higher rates of shingles cases for us. And this may be the case until all of our vaccinated children are of elderly age and the virus is considered “eliminated” from the community.
Models are predicting shingles in our unvaccinated (that means us) will initially increase by 30-50%. But, if childhood vaccination rates are high these rates will drastically decrease after 30-50 years when these vaccinated kids are of prime shingles age. (8)
If you’re reading this page you’ve most likely never been vaccinated against chickenpox. The vaccine just didn’t exist when we were kids. Or you may be from a country where they don’t use the vaccine routinely, which nearly all other countries don’t routinely include the vaccine in the childhood schedule.
The UK, for example, doesn’t use the chickenpox vaccine routinely on their children. This is mostly due to the fear of an increased incidence of shingles. However, they also believe getting the chickenpox as young children may be best due to the fact that getting it as a teen or adult can be potentially life-threatening. Basically, get the chickenpox out of the way when they’re young.
These countries are waiting to see what happens over here in North America before they implement the vaccine as routine there. However, by the time we collect the data on whether or not the vaccine greatly reduces the presence of shingles, these countries may be 50 or so years behind the US as far as vaccination with the chickenpox vaccine goes.
Although you may know I’m a passionate advocate for vaccines, those in other countiries do have some valid arguments against using the chicken pox vaccine. However, if we stick with it here in the US, our future generations should greatly benefit.
We will have to just wait and see what happens with our teens and adults in their early twenties when they’ve reached advanced age to be sure that shingles incidence greatly decreases with the use of the vaccine.
My thoughts on this?
Other countries may be smart to use ours as a test subject. However, this vaccine is great and in the next thirty to fifty years we could be nearly free of chickenpox and shingles in North America. It will take time but will be worth it for our children and grandchildren.
As for us, I think we will be more prone to shingles. However, we do have an amazing vaccine to help prevent that.
If you’re over 50 you definitely want to go get the very effective shingles vaccine called Shingrix. It will get your body working hard to make sure you are less likely to get shingles.
We are lucky we have access to a shingles vaccine, which could be our saving grace as we build up the generation of vaccinated children.
And please, if you do come down with shingles, stay home. Not only do you need rest, but you can pass chickenpox on to unvaccinated people who have never had the virus. Do your best to contain preventable disease.
Get your kids vaccinated and if you’re of age, get yourself vaccinated for shingles. Stay home when you’re sick. And always wash your hands!
Cheers!
References:
- Welsby P. D. (2006). Chickenpox, chickenpox vaccination, and shingles.
Postgraduate medical journal, 82(967), 351-2. - Varicella vaccines. (1998 Aug 7). HO position paper. Wkly Epidemiol Rec. 73(32), 241-8.
- Terada K, Hiraga Y, Kawano S. et al Incidence of herpes zoster in
paediatricians and history of reexposure to varicella‐zoster virus in patients with herpes zoster. Kansenshogogaku Zasshi 199569200–205. - Brisson M, Gay N J, Edmunds W J. et al Exposure to varicella boosts immunity to herpes zoster: implications for mass vaccination against varicella. Vaccine 2002202500–2507. [PubMed]
- Thomas S L, Hall A J. What does epidemiology tell us about risk factors for herpes zoster? Lancet Infect Dis 2004426–33. [PubMed]

